Canada’s COVID-19 Strategy is an Assault on the Working Class

Canada is known for caring for all its citizens, through for example universal health care and excellent public schools. What changed?
The Canadian COVID-19 lockdown strategy is the worst assault on the working class in many decades. Low-risk college students and young professionals are protected; such as lawyers, government employees, journalists, and scientists who can work from home; while older high-risk working-class people must work, risking their lives generating the population immunity that will eventually help protect everyone. This is backwards, leading to many unnecessary deaths from both COVID-19 and other diseases.
While anyone can get infected, a key feature of COVID-19 is that there is more than a thousand-fold difference in the risk of death between the oldest and the youngest. In fact, children have much less risk from COVID-19 than from the annual influenza. Considering this, we must do a much better job protecting the elderly and other high-risk groups until a vaccine is available.
As a contrast, children should go to school in-person while we encourage young adults to live near normal lives to minimize the collateral damage from the pandemic. For them, the public health damage from lockdowns is worse than their minimal risk from COVID-19. Following basic public health principles and numerous pandemic preparedness plans, this is a focused protection strategy, as outlined in the Great Barrington Declaration, with accompanying details on how to properly protect the elderly.
Schools and universities are not only critical for education, but also for physical and mental health and social development. It is positive that most Canadian schools are open for in-person teaching, but not all students are attending, even though there is no public health rationale for keeping them away.
To be scientific about it, we must look at Sweden. It was the only major western country that kept day care and schools open for all children ages 1 to 15 throughout the height of the pandemic in the spring. Without any masks, testing, contact tracing or social distancing, there were exactly zero COVID-19 deaths among the 1.8 million children in this age group, with only a few hospitalizations. Moreover, teachers had the same risk as the average of other professions, while older people living in multi-generational homes did not have higher risk if living with children. To test and isolate children and parents are harmful to children and families without serving a public health purpose.
Despite heroic efforts by the public, the nine-month lockdown and contact tracing strategy has tragically failed older Canadians, with 97% of COVID-19 deaths inflicting those over 60. Where it did “succeed” was in shifting the COVID-19 burden from affluent professionals to the less affluent working class.
For example, in Toronto, the incidence rates were the same at the beginning of the pandemic, but after the March 23 lockdowns, detected cases declined in affluent neighborhoods while they skyrocketed in less affluent areas. A similar effect was subsequently observed for mortality (see Figure).
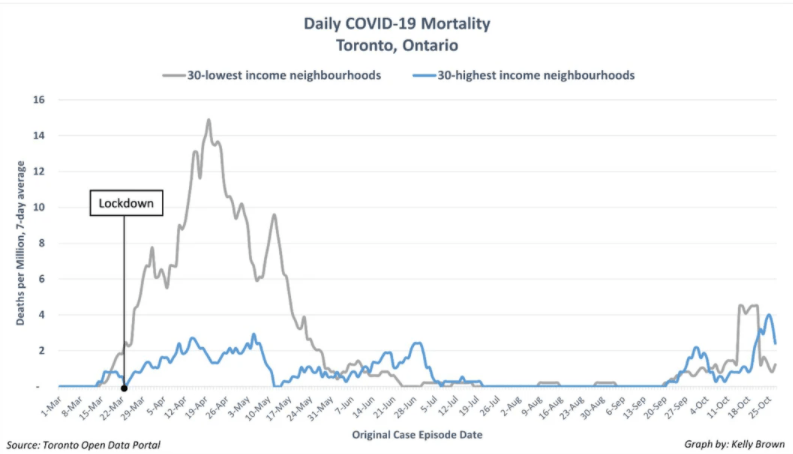
While it is impossible to protect anyone 100% during a pandemic, the notion that we cannot better protect the elderly and other high-risk groups is nonsense. It is not harder to protect the old than it is to protect the affluent, and the former leads to fewer deaths.
Lockdowns have generated enormous collateral damage on other health outcomes, such as plummeting childhood vaccination rates, worse cardiovascular disease outcomes, less cancer screening, and deteriorating mental health, just to name a few. Even if all lockdowns are lifted tomorrow, this is something that we will have to live with – and die with – for many years to come.
One of the basic principles of public health is to consider all health outcomes, and not only a single disease. Having thrown that principle out the window, we urgently need to bring it back to minimize mortality and to maximize overall health and well-being.
Reprinted from The Toronto Sun










