Nursing Homes and Covid Fatalities: The Empirical Relationship

In the search for strategies in dealing with Covid-19, policymakers have preferred broad-based interventions like curfews or business, school, and church closures in order to slow or stop the spread. In the argument over the consequences of these measures, a crucial question has been lost. Where precisely is the greatest risk of severe outcomes from contracting the virus? We’ve known from the beginning of the pandemic that SARS-CoV-2 disproportionately impacts the sick and aged, but what precisely does that imply about policy?
A particularly dangerous setting is Long Term Care Facilities (LTCs). LTCs account for over 100,000 Covid-19 deaths, almost 40% of the total in the United States. To better understand the variance in outcomes across the country, I looked at differences in state-level deaths per capita as reported by the COVID Tracking Project versus the number of LTC residents in each state.
The share of a state’s population in such facilities could be a better predictor of severe outcomes from the virus than nonpharmaceutical interventions such as curfews, closures, and mask mandates. State case and death totals in nursing homes, as they are often reported, give an impression of how deaths are spread across the country. But those data typically do not include a population adjustment, and do not allow for comparisons between states based on their population’s vulnerability.
Vermont and North Dakota both have relatively small populations, 624,000 and 762,000, respectively, and the median age is substantially higher in Vermont. However, North Dakota has more than twice as many people in nursing facilities as Vermont does. States report LTC deaths differently from each other; in New York, for example, deaths in LTCs are undercounted, as staff and residents who die after being transported to a hospital are not counted as part of the total. State outcomes are only comparable to the extent that the data are reported the same way.
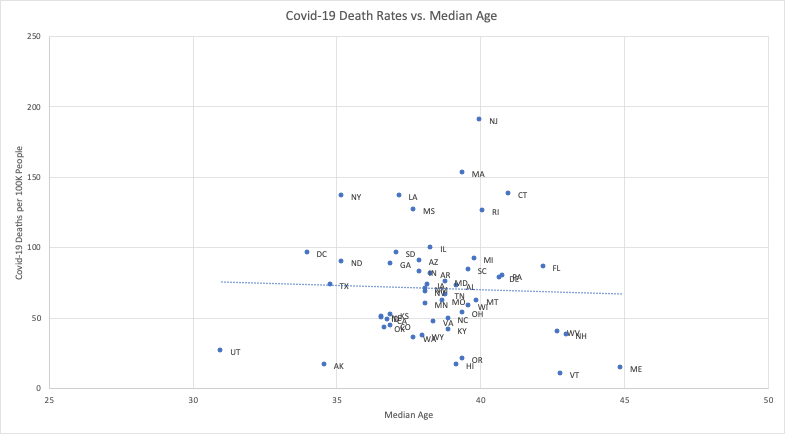
One obvious difference to look at is the median age in each state. However, plotting each state’s median age against Covid-19 deaths shows no peculiar vulnerability (see Chart 1). If anything, there is a slight negative correlation (not statistically significant) between a state’s median age and its Covid-19 death rate. How is this possible? Median age is different from the number of vulnerable aged people in a state. To focus on the most vulnerable requires looking at nursing home populations.
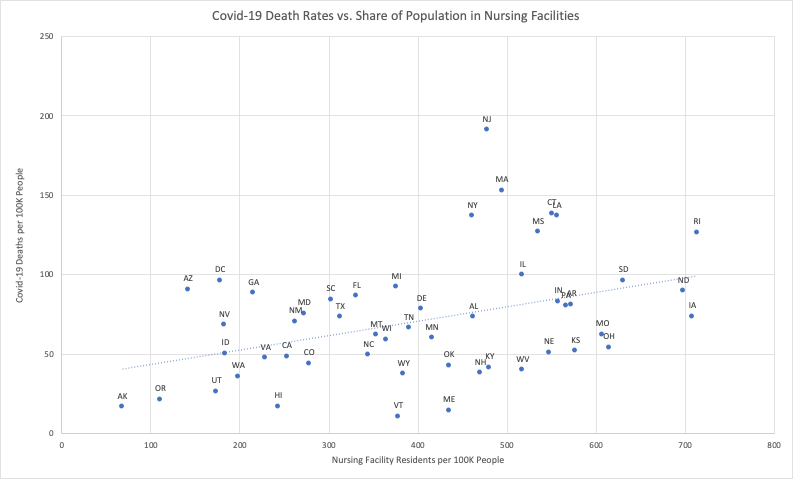
I gathered data from each state and correlated Covid-19 deaths per 100,000 people with the relative size of the population in Certified Nursing Facilities, as estimated by the Kaiser Family Foundation. How do population-adjusted deaths correlate with the state-by-state ranking of numbers of long-term care facilities? The results are noisy, but more conclusive than is seen with many NPIs or by looking at each state’s median age, showing a clear positive relationship between the two measures (statistically significant at the 1 percent level).
What does this imply for public health? Primarily, we should focus on the key objective: protecting the elderly and the sick in these homes from the virus. We’ve known since March that Covid-19 was a problem in these facilities. Why did governors require nursing homes to readmit these patients who were still testing positive for Covid-19, instead of protecting LTC residents from that risk?
Why were they so anxious to shut down schools and concerts attended by healthy young people — or just healthy people in general — while disregarding a vastly greater and more obvious risk? Instead of demanding stricter rules for everyone, governors should look to improve safety in nursing homes.
The data further suggest that certain states continue to have challenges ahead; namely those with a large share of residents in nursing homes. In particular, Iowa, Missouri, Ohio, and the Dakotas need to focus intensely on these institutions.
While not all deaths are preventable, we have a moral obligation to engage in focused protection rather than continue one-size-fits all approaches to public health. To the extent that resources for testing, vaccines, health care worker time, and federal grants are scarce, they should be focused on the most vulnerable, and few are more vulnerable than nursing home residents.










